Editor’s note: This article features key highlights from Oliver Wyman’s recent report about COVID-19's impact on long-term care in Singapore. This report was developed in collaboration with the Lien Foundation. Read the full report here on OliverWyman.com.
Singapore’s management of the COVID-19 crisis resulted in one of the world’s lowest death rates – 28 COVID-19 deaths to date. Outbreaks in long-term care (LTC) also remained very low, but this came at the price of strains on the country’s LTC system. In nursing homes, residents suffered from a halt to visits, while staff had to live in temporary accommodations. Daycare centers were closed for several months, disrupting seniors’ physical and mental health routines and increasing the burden on primary caregivers at home. Homecare stepped in to fill the gaps amid the crisis. COVID-19 has compromised the stability that is imperative to the sector.
As traditional LTC operators scrambled to respond to COVID-19 challenges, they adapted services, operations, and manpower with an inevitable take-up of technology as a solution. These necessary adjustments to fight the pandemic is a silver lining – a catalyst for a “better normal” that puts seniors at the center of care, enabled by digital and technology. Oliver Wyman research – drawing insights from nearly 50 secondary sources in Singapore and other countries – shows how these innovations can help create a future for LTC in which aging-in-place is the default, and which places a renewed emphasis on quality of life. Diverse care options can be administered at home and seniors can be offered a blended program of online and offline daycare services. The report calls for a major transformation across the LTC sector, with a key role for digital technology.
Exploring COVID-19's Impact on Singapore
Singapore makes a compelling case study for the possibilities in LTC care. Singapore is the world’s second-fastest aging country, after South Korea, and 22 percent of its population is above age 60 today. Given this trend, the country has steadily increased capacity in LTC over the past decade. Moreover, the country’s LTC system had a relatively good record during the pandemic, with only four deaths linked to nursing homes and no cases or deaths in daycare and homecare to date. As of October, 46 percent of COVID-19 deaths across a sample of 21 countries was linked to care home residents, and Singapore had the second-lowest number of care home deaths as a percentage of total care home residents.
Today, LTC is physical and high-touch, so the pandemic has posed serious difficulties. Of the three major care segments, nursing homes were disrupted in almost every aspect. Visits stopped and communal spaces were split up for safe distancing, with staff working longer shifts to provide coverage in the new environment. Large numbers of them are foreigners who live in crowded on-site dormitories or off-site residences with one another, and many had to change to different accommodations and adhered to split zones beyond the nursing home walls to avoid virus transmission.
Daycare centers were closed for three months, and many operators scrambled to migrate online for the first time, from basic check-ins to exercise and arts and craft classes. Results were mixed, due to lack of preparation, many seniors’ inability to connect to the Internet, and the unavailability of caregivers at home. But these online trials pointed the way to opportunities for virtual care. Homecare, in contrast, had a major inflection point. Providers in the study saw home nursing grow about 20 percent and home medical care between 25 and 50 percent. Operators also piloted telemedicine services – from doctor calls to medicine delivery – during COVID-19, indicating a promising foray into virtual care delivery.
The Evolution of LTC
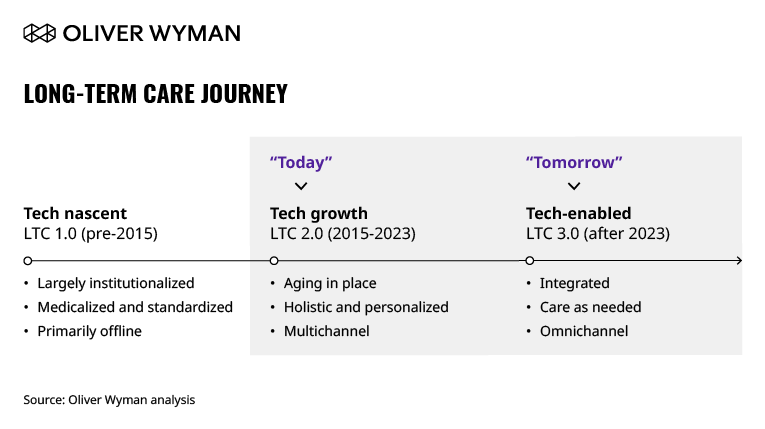
Prior to the pandemic, LTC in Singapore has been evolving in response to the growing demands and changes in preferences of its aging population. Just a decade ago, seniors found themselves in highly medicalized, custodial forms of care – LTC 1.0 – with dozens of residents packed into one bedroom and practices such as physical restraint. Since then, under LTC 2.0, more aging-in-place options have emerged: Integrated home and daycare services launched; “Kampung Admiralty”, a senior-friendly public housing, opened its doors, recreating sentiments of traditional community-living; and homecare tech platforms, such as Jaga-Me and Homage, entered the sector, bringing convenient care into people’s homes.
COVID-19 challenges accelerated the path for a further shift forward – while we are not there yet, we are edging towards LTC 3.0. In this model, seniors will seamlessly move across care and service settings – both online and offline – and receive care only as needed. Digital technology will play an amplified role, boosting choice, ensuring access to care, and increasing efficiency. Aging-in-place will be the clear default, meaning that greater numbers of people can receive quality care and live more-normal lives for longer.
Getting to LTC 3.0
To move from these trials towards LTC 3.0, operators should first prioritize immediate gaps in their services. We have identified six actionable opportunities where pilots are already emerging in Singapore. They leverage practical, technology-based solutions that are already being applied and have proved especially effective during the pandemic.
- Pivot to digital-led care models that are integrated closely with offline models. Examples include telehealth, using remote monitoring and back-end analytics, and virtual daycare.
- Boost preventive health and wellness. Empower patients and plan for future disruptions by deploying sensor-based technology such as wearables and remote devices for medication adherence.
- Retrofit existing spaces in facilities to minimize the risk of infection. Redesign nursing homes and daycare facilities and introduce devices such as assistive robots and AI-based solutions (software for CCTV facial recognition and temperature screening, for example).
- Empower the workforce for the future. Use lessons from COVID-19 to redesign jobs and reorganize teams; engage and upskill volunteers; free up staff using technology such as remote monitoring, IoT-enabled administrative systems, and assistive robots.
- Place greater emphasis on mental health and wellbeing in care planning. Focus on social connectivity through digital platforms and VR-based programs.
- Provide greater support for primary caregivers via upskilling and wellbeing initiatives to better prepare them to navigate uncertainties. This can be done through digital communities and training for caregivers.
Transformation Lessons from Other Industries
Care providers can learn from other industries – such as insurance, banking, and hospitality – that have used digital technology to fundamentally transform their propositions and operating models. These shifts have ultimately helped better address the underserved needs of different populations – for example, digital banking for the underbanked. One principle for sector incumbents is to challenge the status quo. In LTC, that means swapping a medicalized model centered on dormitory-style nursing homes and fragmented care sites for a one-stop hub in every single neighborhood – from primary care to daycare – both online and offline care. Seniors can truly remain at home independently, and digital tools will carry out passive monitoring so that people will receive care only when needed.
Rather than waiting for a big-bang transformation, LTC operators should pursue rapid, incremental innovation, testing, and iterating solutions quickly. Some providers did this successfully during the pandemic, rolling out new services such as online activities and telemedicine. An effective way to develop new services is through partnerships that leverage the comparative advantage of other sectors and partners, such as quickly engaging Regional Health Systems and private home care providers to train staff across care facilities to perform swabbing. Operators should proactively identify areas where they can leverage such cooperation. An essential principle is to start viewing seniors as consumers rather than patients, taking a design-thinking approach to re-orient new digital programs and tech solutions to end-users.
A Whole-of-Sector Approach
Though individual operators must first push ahead with their own innovations, the transformation to LTC 3.0 will only succeed through a whole-of-sector approach. The government will drive many of the structural enablers, such as financing for telehealth and digital-health solutions beyond the COVID-19 crisis. In Singapore, for example, the Ministry of Health is responsible for policymaking and much of payor coverage, while the Agency of Integrated Care coordinates long-term care operators. Hence, these are important players for the constant sharing of best practices and other knowledge across the sector.
Other players, such as corporations, tech partners, and academic institutions, can provide financial and technical resources that the public sector cannot supply itself. Corporates have supplied volunteers, as well as provided funding to fill in gaps such as new beds for nursing homes’ staff dormitories. They will continue to bring the financial resources, tech, and innovation to drive changes beyond what the public sector can spur on its own. Operators will contribute to the system by serving as the key communication channel between seniors and their caregivers, on the one hand, and policymakers and other stakeholders, on the other.
COVID-19 has upended normal life and has disproportionately impacted older adults. But the pandemic’s silver lining is the momentum for change and digital adoption.