KEY TAKEAWAYS
- Leaders must think about innovation like they’re building a home from the ground up.
- Many leaders default to spending all their time and resources in the “performance” and “productivity” zones, missing the vital innovation and potential new business opportunities found in the “incubation” and “transformation” zones.
- Working across multiple zones requires leaders to develop different competencies and redesign metrics to measure success.
Finding a show that my whole family enjoys is no easy feat. I love heartwarming tales where heroes overcome challenges (Outlander, minus the violence). My husband loves dark, ironic dramas (Breaking Bad, anyone?), and my kids love cartoons, mostly mindless ones. So, we were thrilled when we stumbled across Grand Designs, a British home renovation show featuring people who restore older buildings and transform them into the homes of their dreams. All of us love it. We especially love the “before” and “after” aspect, and seeing how people choose to protect or preserve certain elements of the original building, creating something new and purpose-built for their family. We suddenly fell in love with the idea of renovation. Then we lived through our own.
Both Simon and I independently undertook pretty ambitious home renovation projects over the past year, and in parallel worked closely with payer and provider clients striving to transform their businesses and create something purpose-built for a new set of needs – while protecting and preserving what was important from the legacy business. We were struck by the parallels.
It’s not easy to seamlessly incorporate new building materials, new plumbing, and new technology into old buildings. But this must be achieved if you want your dream home manifested.
We talk to many chief executive officers who have the same dilemma when trying to deliver their own “grand designs.” How do they make the very best use of what they have now while ensuring they’re up-to-date with the latest innovation? It’s easy for healthcare leaders to get caught between risk and return, often bounded by the need to deliver on operational metrics. Why risk changing the status quo – or, worse, spend already limited dollars on something unproven? The pace of disruption is hard to predict, and it’s difficult to extrapolate the future from the past when it comes to innovation. As a result, most organizations tend to avoid doing anything for a while, choosing to wait it out. Afterward, though, they may be forced to take big, risky actions that come too late.
To thrive during this volatility and create resilient organizations, healthcare leaders need to create new “grand designs.” Thinking about innovation like you’re building a home – which is both a challenging and opportunistic undertaking – can help leaders identify the new mindset, skills, and priorities needed to prepare an organization to seize tomorrow’s opportunities.
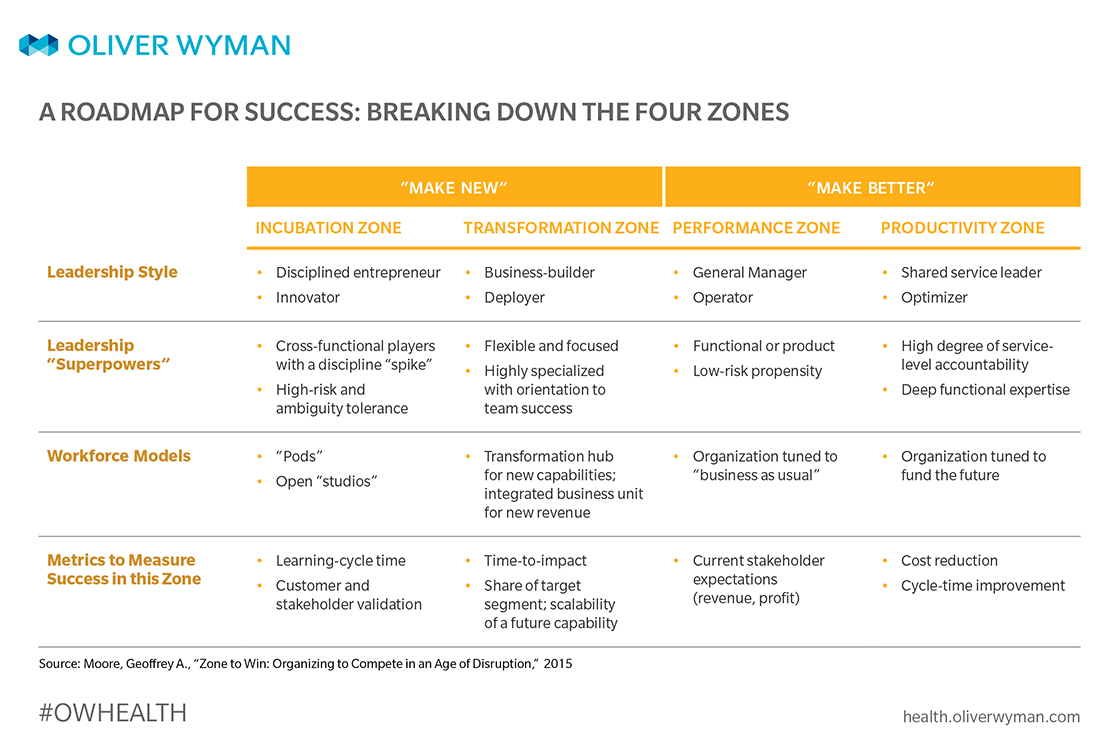
Consider the following four design zones, inspired by Geoffrey A. Moore's book, Zone to Win: Organizing to Compete in an Age of Disruption.

BUILDING INNOVATION FROM THE GROUND UP
Building on Geoffrey Moore's four-part framework, here are some targets of ways to allocate management time, attention, and energy, and some examples of successful healthcare initiatives within each zone.
1. Performance Zone (Target: ~ 40 percent) – Most leaders tackle performance management by focusing on profitability. It may be about protecting market share in key product areas like Medicare Advantage or clinical service lines, or improving medical cost management for specific populations. They’re also addressing growth and positioning – to ensure the right consumers are targeted with the right message and the right product offering. Likewise, they want to optimize the credential and referral processes. In some cases, that involves monetizing services to the marketplace – for example, when medical directors who monitor the effectiveness of drugs use that capability to advise employers on formularies.
2. Productivity Zone (Target: ~ 30 percent) – Since efficacy and efficiency is the main play here, leaders in the immediate term use medical management to drive costs in a meaningful way. Longer term, they’re using game-changing capabilities (like artificial intelligence) to reduce prior authorization or enhance throughput of radiology. Productivity enhancement requires a relentless eye on what’s driving cost and how it can be brought down. At the same time, it means every player is performing the highest value tasks they’re most qualified to do with an eye towards patients seeing the appropriate clinician in the most suitable medical facility at the right time.
3. Incubation Zone (Target: ~ 20 percent) – As an example of successful incubation, a regional health insurer partnered with a large media telecom company to launch a joint venture at the intersection of their industries. The new company connects consumers and providers on a specific care path. Imagine longitudinal care in the home where all members of the family and care team can communicate, where technology in the home monitors people’s conditions and provides prompts when medical emergencies are imminent, and where patients are empowered and informed to manage their conditions at home.
4. Transformation Zone (Target: ~ 10 percent) – An example of companies embracing transformation includes payers who retool their network to focus on low-cost access. Another instance is a large regional health plan redefining its insurance product by contemplating multiyear subscriptions, freeing them to invest in population health programs that don’t necessarily yield in-year returns.
When leaders face disruption on so many fronts, understandably many default to spending all their time and resources in the “performance” and “productivity” zones. These two zones are critically important because they make an organization better. But leaders who only spend time in those areas miss the vital innovation and potential new business opportunities found in the “incubation” and “transformation” zones.
To deliver their new “grand designs,” leaders need to rebalance and allocate the appropriate level of energy, attention, and financial investment to build a portfolio across all four zones and create a resilient organization that can nimbly respond to future challenges and opportunities.
Of course, with this all being a little new, healthcare executives must excel in multiple zones by developing different competencies and redesigning metrics to measure success.
EXHIBIT 1
FIVE WAYS TO GET STARTED BUILDING YOUR OWN “GRAND DESIGN”
1. Start early and take small bites towards the future business. To lead across the four zones and build the organizational muscles for this new mindset requires time and resources to change an organization’s operational model, behaviors, and ways of working. It’s a long journey, one that requires significant resources. Starting sooner in a small way is better than delaying completely because of cost.
2. Embrace leadership as a team sport. Change, neither quick nor easy, involves thinking about leadership in completely new ways. This means letting go of the traditional command-and-control structure and shifting towards developing strategies for leading multidisciplinary teams that may include both company employees and a more dispersed workforce that contributes through crowdsourcing and other open platforms.
3. Rethink promotion and succession. So many healthcare executives rise through the ranks as specialists. Actuaries become executive vice presidents of products or even chief executive officers of insurance companies because that specialty was critical to the success of the business. Other chief executive officers come from backgrounds in government regulations at companies where they need to woo regulators. In hospitals, chief executive officers are often medical doctors first. Healthcare leaders can take a page from other industries like retail or consumer packaged goods, where the chief executive officer rotates through several functions from branding to marketing to manufacturing, then runs a profit- and-loss unit before ultimately leading a company. Leadership training in healthcare should become broader to develop skills across various functions. Design management teams to include a diverse array of executive backgrounds.
4. Consider new C-suite roles. A stand-alone chief data, analytics officer, or head of innovation can help companies think across our four zones as they drive technological advances, explore and implement new technologies, and upskill the workforce as technologies like artificial intelligence, robotic process automation, and virtual care become more prevalent.
5. Incorporate empathy-based design thinking training throughout the organization. Healthcare continues to become more consumer-centric as consumers increasingly make more decisions about their own healthcare, from choosing providers and health plans, to Googling their symptoms, to seeing a doctor at their local drugstore rather than at their primary care provider. Empathy-based, design thinking at all levels can help organizations embrace this consumer-first mentality.
With this roadmap in place, you’re set to begin your company’s transformation. As we both realized watching scores of Grand Design episodes, whenever a new home is complete, it looks and feels amazing (and, funny enough, the pain of getting there suddenly doesn’t seem as vivid). Similarly, payers and providers who mindfully “renovate” their companies based on Moore's framework will have competitive advantage by being well prepared for emerging needs, while still safeguarding their most important legacy business aspects.
For more Oliver Wyman Health insights, visit health.oliverwyman.com.
ABOUT THE AUTHORS
- Simon Holland, Partner, Organizational Effectiveness, Oliver Wyman
- Helen Leis, Partner, Health & Life Sciences, Oliver Wyman

