Our April workshop was a great success. With our Roadmap to 2025 in place, the Oliver Wyman Health Innovation Center (OWHIC) teamed with more than 20 healthcare leaders to capture the best new thinking on how to implement patient-centered care at scale. (The full agenda can be found here.) The group learned how to implement the best clinical models, avoid critical mistakes in building infrastructure and new competencies, and debated the optimal paths for organizational and financial migration. With our advisors co-facilitating, we also brainstormed how to create a consumer and employer market for population health management – a market where population health models are chosen over open-access PPOs. The session included senior leaders from across the healthcare spectrum: health plans, health systems, capital markets, HIT, and emerging technologies. Their work demonstrated the impact of collaboration and the need for the industry to rethink the existing compete/collaborate framework. Here are some takeaways from our attendees:
Tsunami of tools coming 2 facilitate #patientengagement in #health issues & care plan predicts @bcbsla CEO Mike Reitz bit.ly/1017twz — Oliver Wyman (@OliverWyman) May 15, 2013
Clinical, IT & ops need active dialog to move in same direction, says @cornerstonehcnc's @gracet22 #carecoordination cot.ag/TKdJpy — Oliver Wyman (@OliverWyman) May 15, 2013
@mckesson_mhs Pres. Emad Rizk: When commercializing product, pick partners carefully to align incentives & ensure trust #OWHIC #pophealth — Oliver Wyman (@OliverWyman) May 14, 2013
@deancare CEO Samitt on shift to value: Start w/ top 5 diagnoses w/ respect to spend, then invest in rest of pyramid cot.ag/15tTGGG — Oliver Wyman (@OliverWyman) May 10, 2013
For more on the ongoing work of OWHIC and
its bold vision, see Clinical Innovation + Technology's
July 2013 cover story "All Rise With Innovation."
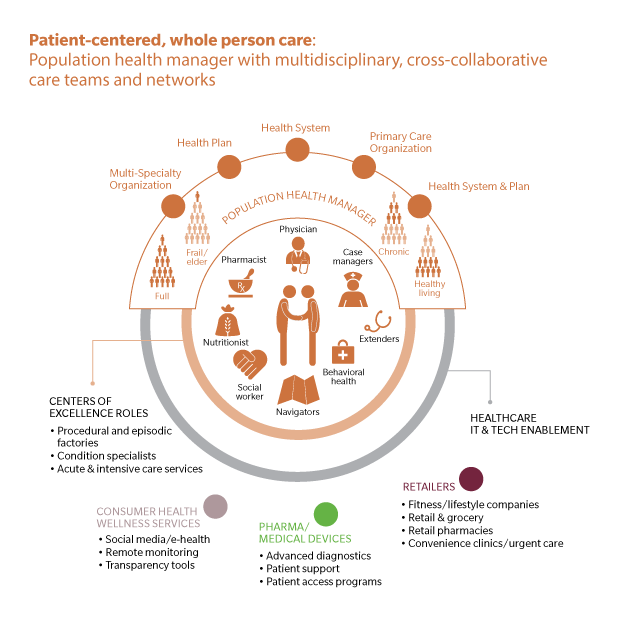
Patient-Centered, Whole Person Care
A highlight of the event was a visit to CareMore, arguably the best population health management model for frail elders in the U.S. – and a model that has already been brought to scale, replicated, and successfully expanded into many new markets. Leeba Lessin, EVP and President of WellPoint Medicare Programs (CareMore’s parent), graciously hosted us for a “best practice” tour, providing an amazing springboard for our workshop and a starter set of ideas on scaling patient-centered care.
Changing the existing paradigms in healthcare will require a fundamental shift in thinking – away from transactional care for sick patients to preventive care aimed at the whole person. This requires a patient-centered approach that considers the patient’s unique needs and tailors a treatment plan aimed at preventing disease progression. Just like at CareMore, patient care will extend beyond the clinic into patient homes and lifestyles through multidisciplinary care teams utilizing connected networks and wired, intelligent devices that support treatment adherence and generate ever more personalized care regimens.