Thirteen of the 32 Pioneer ACOs met their savings targets and received $76 million in shared savings payments from CMS, the agency stated. Another 17 saved money, though not enough to qualify for shared savings. Two lost money. Are those good numbers or bad? Is Pioneer ACO succeeding or failing? In this client briefing, two of Oliver Wyman’s most experienced ACO builders interpret CMS’s report in light of what ACO Pioneer aims to accomplish — and their own understanding of the life cycle of the ACO.
The Path to Value: A Balancing Act
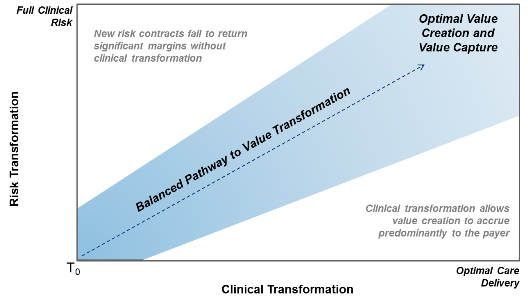
Can value-based care really solve the U.S. healthcare crisis? We believe so, but the path to value requires a careful transition in both care delivery and provider reimbursement. If healthcare providers take on too much financial risk and are unable to balance it with improved quality of care and better outcomes, they will suffer financially. (That is more or less what happened to the HMOs of the 1990s.) On the other hand, if they transform themselves clinically and don’t take on risk-based arrangements, the financial benefit of transformation will all go to payers — much to the detriment of the providers.
Pathway to Value Transformation
Source: Oliver Wyman







