Editor’s Note: The following article is part of an ongoing series offering our strategic advice and expertise on what healthcare industry stakeholders should do immediately in response to the rapidly evolving novel coronavirus (COVID-19) pandemic.
Hospital bed capacity. Three words the healthcare industry is urgently struggling with amidst the COVID-19 pandemic. In especially hard-hit countries like China and Italy among many others, already stressed hospitals have been experiencing a surge in patient demands. To date, there have been over 5,200 confirmed reported cases as of now across the US. This is a surge our healthcare systems are unequipped to handle.
Clinical evidence shows that most – 80 percent – of COVID-19 patients will experience only light to moderate symptoms (like a cough and moderate fever). Providers must develop clear solutions that enable patients to effectively manage their care at home, and monitor their status with their provider.
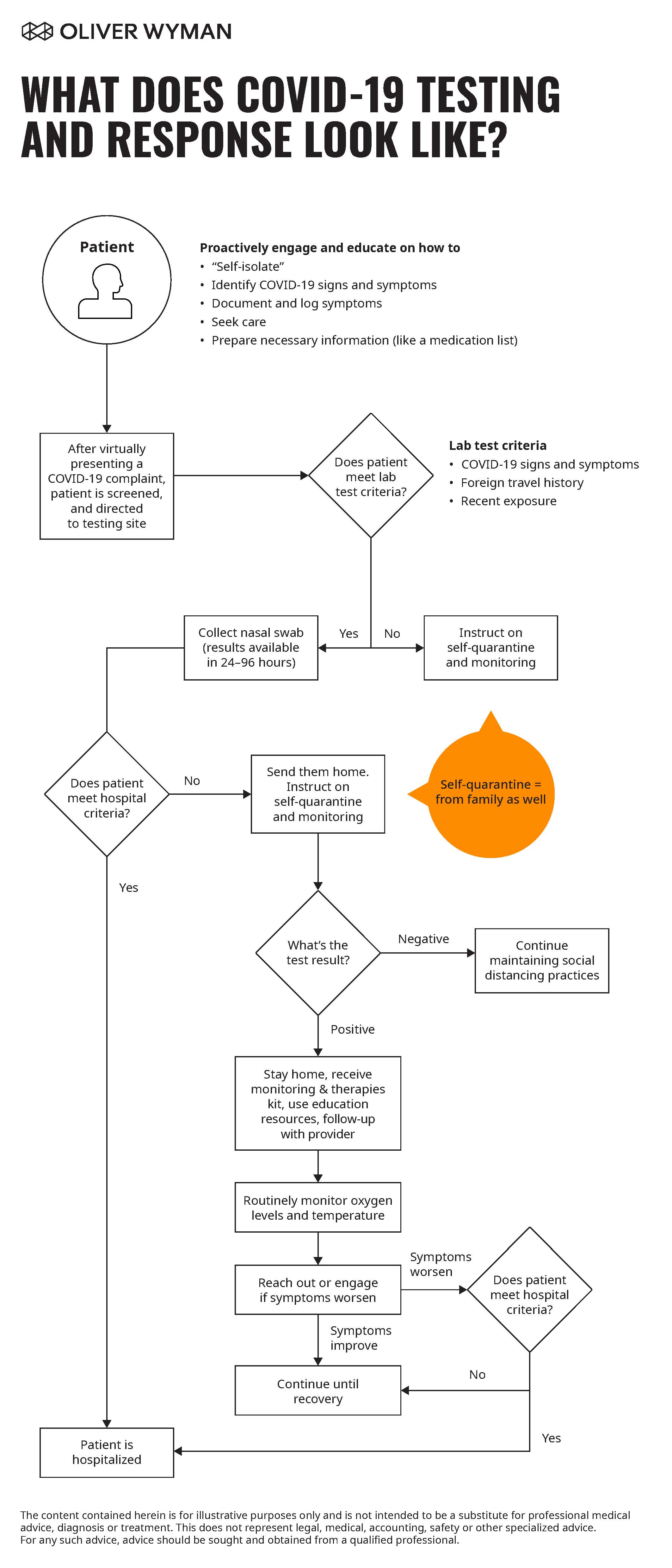
The Patient Journey: From Symptom Onset Through Home Monitoring
Providers are monitoring infected patients for exacerbations while seeking to maintain available capacity to admit patients in need of hospital-level care. To solve this challenge, providers must consider leveraging off-the-shelf technology and creating a remote monitoring workflow that enables and guides patients through self-monitoring and on to their recovery process.
Here are some urgent action items to follow now to ensure your patients are directed to the right place at the right time.
First, providers should proactively reach out to their patient populations. Special attention should be paid towards connecting with particularly at-risk populations. These patients include those 60 and over with multiple co-morbidities like congestive heart failure, chronic obstructive pulmonary disease (COPD), diabetes, and heart disease, and the immunocompromised. The following information must be shared with all patients, including:
- How to “self-isolate” – including from people in their own household
- COVID-19 signs and symptoms and how-to self-document an onset of symptoms
- How and when to contact a healthcare provider (for example, if someone should reach out virtually first)
- What documents they need to have on hand when contacting their provider (like a medication list or documentation of signs and symptoms)
- The importance of designating a family member or loved one as a primary caregiver when possible. Family caregivers should also be contacted and provided the same educational materials
After screening these patients, providers will direct individuals of COVID-19 to a testing site. COVID-19 testing guidelines are evolving rapidly as testing capacity is increasing. These guidelines will likely continue to include travel history, fever, respiratory symptoms, recent exposure to a COVID-19 patient, prior medical history, and a medications list.
Even before testing begins, people with symptoms of moderate or severe disease may be directed to an acute care facility appropriately equipped for isolation and care of COVID-19 patients.
Screening and testing sites should be separated from existing care locations. Many providers are now building tents in hospital parking lots or in drive-throughs facilities to reduce the risk of infecting other patients. When a patient arrives at the screening site, a clinician wearing Personal Protective Equipment (PPE) will re-screen patients and collect a nasal swab to test for COVID-19. Additional triage using simple lab tests like white blood cell counts (WBCs) and x-rays may help determine if hospitalization is needed.
Although more labs are being brought online to handle COVID-19 tests, current turn-around times for test results are expected to take at least twenty-hours. The implication is that most patients must be sent home with materials and instructions for self-monitoring and detailed instructions on how to conduct self-quarantine as they await results.
People awaiting screening results should be isolated from other household members. They should also avoid leaving their homes. Recent data from China show a 14 percent rate of intra-family infection from an infected person. In response to this issue, some countries have established monitoring centers so patients avoid exposing their families.
As test results arrive, patients who have tested negative should continue to practice social distancing. They should also continue practicing other related hygiene routines. Patients should therefore be reminded to continue to look for symptoms in themselves and in family members, and to seek further advice should these appear.
Positive patients should be sent a support kit with educational materials, monitoring tools (such as a thermometer and portable PaO2 monitor to measure their oxygen levels), and medicine to help alleviate their symptoms.
A positive result is likely to cause significant anxiety for the patient, their loved ones, their family, their workplace, and beyond. A key task for providers will be to educate patients on disease progression, complication risks, and best practices for self-care during a difficult time. The patient should be connected to their primary care doctor for this advice or remotely engaged with a home health clinician. The family member’s caregiver should be notified and given similar instructions as well.
Most patients should be able to overcome the infection at home without hospitalization. Patient education is key. Educational information such as written materials, online videos, and call center support are some additional examples of resources patients should be able to access to educate themselves and alleviate concerns.
COVID-19 symptoms can be monitored at home with simple tools and steps: a thermometer and a pulse oximeter are cost-effective, easy to operate, disposable, and easily delivered. Patients should be directed to periodically self-monitor their symptoms, such as temperature and blood oxygen level. As symptom values cross certain thresholds, clinicians can be alerted and can then contact the patient as needed. The patient can then be assessed remotely. Then, a decision can be made to direct them if needed to a physical location for further evaluation.
We understand what we’ve described is not the situation for all COVID-19 patients, especially those who are unable to get tested or for those whose local health systems lack adequate supplies. With proper education, careful monitoring, and simple telehealth tools, health systems can use limited inpatient care capacity judiciously while ensuring their broader patient populations are recovering from less severe COVID-19 infections.