COVID-19 has forced health systems to dramatically step up the pace of decision making and organizational agility practically overnight. Decisions that may have previously taken weeks or months to execute suddenly needed to be completed in mere hours. The volume and scope of daily decisions multiplied several times over, often forcing traditionally siloed units to come together in uncommon ways.
Now, as we look to what the next half of 2020 may bring, leaders face a long road ahead with monumental challenges, including maintaining surge preparations, safely delivering COVID and non-COVID care in parallel, and recovering from a financial crater in their budgets. Many health system leaders remain hopeful their recently gained agility will be sustained and used as a competitive advantage to navigate challenging times ahead.
On that note, below, we consider four operating model lessons from the early crisis and consider how leaders might sustain and build on their newfound agility.
1. The power of a unifying purpose was on full display.
The pandemic created and continues to create a unifying purpose that drew out a near-universal willingness to help in any way needed to meet this unprecedented challenge. Departmental politicking dramatically subsided, and people at all levels banded together to find creative solutions to shared problems. This phenomenon was even seen in academic institutions, which have historically faced especially challenging silo dynamics.
We’ve learned from COVID that health systems can move with more speed and intention with better alignment on the purpose, vision, and strategy. As systems continue to manage through COVID, communications that continue to win hearts and minds through clarity of purpose and direction will help clinicians and staff fight through the fatigue and collaborate effectively. When the pandemic eventually subsides, formalizing and diligently championing new “thematic goals” or “wildly important goals” can serve as new rallying cries to all to achieve a common objective.
2. Risk tolerances changed almost overnight.
Health systems are usually more risk-averse organizations operating on consensus – features often credited to a high focus on patient safety (“First do no harm.”) and to the slow and careful scientific training of clinicians. The pandemic brought a high degree of urgency and uncertainty driven by the rapidly developing science that made the status quo untenable. Delays would put lives at risk, so decisions had to be made with incomplete, imperfect information – and then quickly implemented.
Whether it was building new partitions to segregate COVID patients, imparting COVID-specific workflows into the electronic medical record (EMR), changing long-established care protocols, or meeting other pressing needs, needed changes were quickly implemented organization-wide. If the first solution didn’t work as expected, teams adapted. The urgency of the situation forced a far higher level of acceptance that failure and iteration would be part of the process.
This highlights the value of cultivating a culture and organizational risk tolerance that favors learning and continual improvement without compromising safety, as well as a management bend to action and iteration over perfect planning.
3. Management transparency combined with local delegation to foster accountability.
Follow-through from ideation to implementation dramatically improved under heightened management focus, transparency, and communications. Leadership teams across the organization were meeting daily to assess key issues and progress. Various organizations were holding organization-wide calls or webinars multiple times a week with clinicians and staff to share priorities and perspectives as they were evolving in real-time.
Many also delegated and pushed decision-making authority to the front-lines, empowering facility and department-level leaders to make critical process changes in real-time. This cut out “red tape” and sped up the pace of change, but also naturally led to some confusion from variation in approach across sites.
The intensity of coordination seen under a crisis is not practical in normal times, but there are ways to foster robust execution follow-through with leaner approaches. Enabling local teams with the right data and analysis, encouraging and supporting innovation within clear boundaries, and defining and transparently reporting success metrics will all help ensure stronger ownership and better execution.
4. New clarity emerged about our understanding of what work is essential.
The pandemic created a singular focus on a narrow scope of activities – preparing for and caring for a surge of infectious disease patients. Most other tasks and projects not directly contributing to this objective were put on hold, including long-term strategic projects. This has highlighted the power of organizational focus, but strategic projects must eventually resume and there will be fewer resources available to support them. As leaders consider how to maintain agility for future success, one of the biggest risks is in allowing a broad return to past ways of working. We have seen that work can be done in very different ways. Capitalize on this opportunity to reevaluate what work is truly essential and how ways of working may be improved to build back better. Identify the value-add tasks (and work locations), automate or streamline them, and eliminate all other task burdens. This increases team bandwidth and creates a funding pool to reallocate into the enterprise to ensure sustainability and reinvigorate growth.
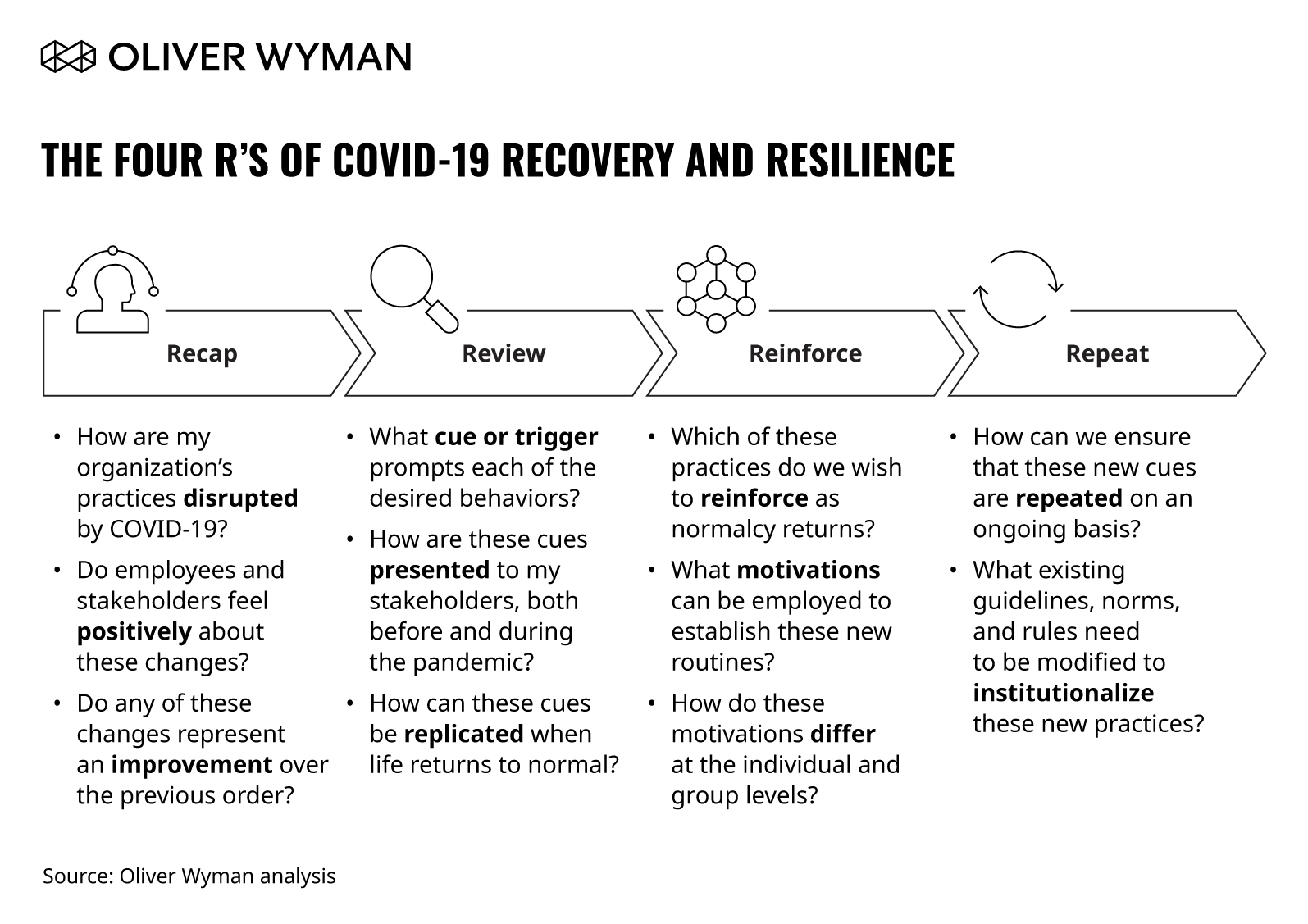
As organizations assess how ways of working have already been disrupted and consider what to embed and sustain ongoing, consider this four-part framework for recovery and resilience:
While the intensity of focus seen during a crisis is not practically sustainable, there are ways to sustain rapid decision-making with robust and immediate execution using leaner and rapid cycle approaches. With the industry changing at unprecedented speed, applying the lessons learned will become the critical success factor health systems need to sustain themselves in the future.