The impending rise of Trumpcare, along with the nomination of Rep. Tom Price to lead the Department of Health and Human Services, has been interpreted by many in the industry as a direct shot at value-based programs like Accountable Care Organizations (ACOs) and bundled payments. Given the changing political winds, some healthcare organizations may be inclined to freeze or retreat from their value-based efforts.
This would be a mistake, says Oliver Wyman’s Josh Michelson. Here, he explains why; and he shares his thoughts on how organizations can get impact from value in the age of Trump.
Why value-based care is still relevant
Regardless of the political landscape, the fundamentals of fee-for-service healthcare continue to erode. Currently, most health systems rely on cross-subsidization economics – where commercial patients often cover 140+ percent of costs to mitigate losses from Medicare and Medicaid, according to Oliver Wyman analysis. But a number of factors are making this Robin Hood dynamic harder to sustain, even for systems with a healthy payer mix:
- Inpatient utilization – the core economic driver for hospital systems – is deteriorating, as care shifts to outpatient settings.
- Medicare and Medicaid coffers are still shrinking, putting increasing downward pressure on pricing for these segments.
- Consumer out-of-pocket spend is rising. In 2016, more than 50 percent of people with commercial insurance had a high deductible health plan, and getting more consumers to have “skin in the game” is a goal of the new administration.
- Republican proposals to eliminate the ACA’s individual mandate, halt Medicaid expansion, and limit Medicaid funding through block grants to the states could have a significant impact on provider economics. A recent report from the Urban Institute suggests that defunding the Medicaid expansion alone will result in a $1 trillion decrease in provider spend over the next decade.
It is clear the need for providers to compete on value – with a lower cost base, better management of medical spend, high quality care, better customer service – has never been more important. For most provider organizations, that means continuing toward value via risk arrangements and ACOs. For institutions that have already started down the road, it means ramping up efforts and more fully committing to the organizational and cultural changes that will enable true population health.
Where value stands today
Understanding why the shift to value has, to date, advanced at glacial pace can help organizations move more effectively and efficiently to value.
Momentum in value-based care has been building over the last several years, and 2016 was no exception. Oliver Wyman analysis shows that:
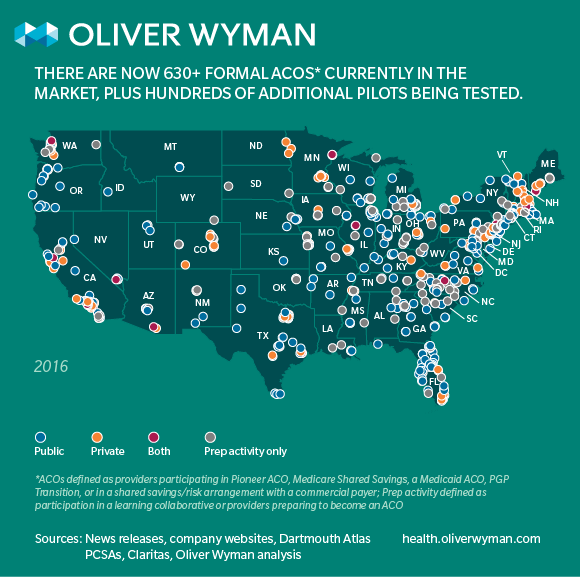
- There are now more than 630 ACOs in the United States
- A majority of residents in almost all 50 states live in a geographic area with at least 1 ACO
While ACO penetration is robust, there is little substantive movement toward value; and the reality is most healthcare organizations are still hovering near the starting line.
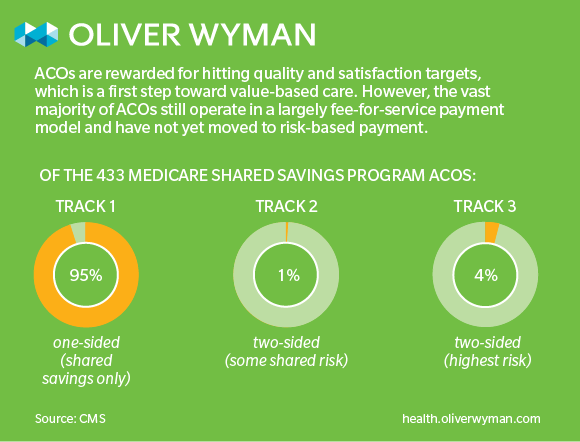
Why? Today’s prevailing value-based payment models do not provide enough incentive to behave differently. The lion’s share of value arrangements – both in government segments and the commercial market – are based on some form of pay-for-performance or gain share. Currently, about 95 percent of MSSP ACOs are in Track 1, which is based on a shared-savings model with no downside risk that effectively shadows fee-for-service, but rewards more efficient care and improved quality. Given the substantive investments associated with a shift to value, most provider organizations have been unable (or unwilling) to justify the spend without accepting material downside risk.
In addition, most providers are struggling to institutionalize a model that runs counter to their very DNA. Many systems are trying to reconcile value-based initiatives with:
- Deeply embedded rewards that center on productivity and putting heads in beds
- Fear of pressing the physician community to change and reluctance to become transparent about individual cost and quality performance
- Siloed acute and ambulatory medical group operations and P&Ls
- Uncertainty around the enterprise-level financial ramifications during the transition period
Finally, there is the reality that demand for value remains uneven. Government-sponsored ACO programs have served as a valuable testing ground, and private payers are often willing to strike value-based arrangements for their government lines of business (Medicare Advantage, Medicaid, Public Exchange). But risk deals around commercial group segments have been a steeper hill to climb. Few employers are willing to disrupt the open-access PPO model, and payers and providers often struggle to find an appropriate price of entry (base rates discounts on fee-for-service).
Without these lives, it can be difficult to achieve sufficient scale.
The way forward
To overcome these institutional and cultural hurdles, systems should focus on these key moves:
Play offense with target populations. ‘Going deep’ on target populations (such as frail elders and people with multiple chronic diseases) with comprehensive care models and substantial two-sided risk can help generate near-term cash flow to fund other population health efforts. It also can help break the pilot mindset and serve as a catalyst for broader organizational transformation.
Invest in organizational change, not just assets and capabilities. Investments in data connectivity platforms, population-based analytics, care coordination initiatives, employee ACO pilots, and the like do not, on their own, generate a clear ROI. These foundational steps must be accompanied with more disruptive organizational change levers, including:
- Redesigning the underlying clinical models of existing practices
- Proactively engaging patients in their health
- Sculpting the physician network such that only high-performing practices or clinicians are able to participate in value-based deals
- Being transparent about practice and physician-level performance
- Redesigning both primary care and specialist incentives to align with population health principles
- Promoting system thinking and economics vs. site of service
Cultivate trust and collaboration between payers and providers. Too often, value-based deals are approached with the same level of antagonism as traditional base-rate negotiations. With the administration’s commitment to value-based payment uncertain, it will become increasingly important for providers to partner with payers on their managed lives; and the time for a new, collaborative approach is now.
Harness innovation to improve underlying health. There is incredible innovation in prevention, health maintenance, lifestyle support, passive monitoring, and engagement; but they are locked out of the $3 trillion dollar sick care marketplace defined by CPT codes. Providers that are able to assume greater levels of risk (percent of premium) can turbo-charge their results through these interventions. But they need to be woven together into health ecosystems. Payers have an important role to play here through new product and benefit designs, as do employers as the ultimate purchasers.
Breaking the gridlock
Regardless of who is sitting in the oval office or at the helm of HHS, value-based care and population health remains the healthcare industry’s future. But breaking today’s gridlock is still an immense challenge. What we have learned from leading organizations is that transformation to true population health can be staged to control costs and organizational stress; that high-impact, early initiatives can help fund additional efforts; and medical staff can not only be retained but reinvigorated by an approach to care that puts patients first.
But it requires true commitment across the whole organization. For organizations that see an essential role for themselves in the future, the time to act with conviction is now.