COVID-19 has altered the fabric of everyday life. Work, education, travel, socializing — all have undergone a dramatic change and may never look quite the same again. Healthcare is no exception. Interruptions to in-person care and the accompanying surge in telehealth adoption are already shaping our experience, behavior, and expectations in lasting ways.
Amwell's annual survey of physicians and consumers offers a snapshot of this inflection point. In addition to affirming the acceleration of telehealth use during COVID-19, the findings reveal evolving attitudes toward telehealth and a new appreciation — on both sides of the virtual visit — for the role that digital technology will play in the delivery of healthcare moving forward.
In last year's survey, just eight percent of consumers had ever had a virtual visit. In 2020 that number shot up to 22 percent — and 59 percent of those patients had their first visit during the pandemic. The increase was even more pronounced among physicians: 80 percent had a virtual visit in 2020, up from just 22 percent in 2019.
The unprecedented number of physicians and consumers using telehealth isn't the survey's biggest takeaway, however. It's how they are using it. They're using telehealth for urgent, primary, and specialty care, on a range of devices, in a variety of settings, and with people they already know.
Historically, urgent care has accounted for the vast majority of telehealth visits. That trend flipped during the pandemic. Just 21 percent of the consumers who used telehealth in 2020 had an on-demand urgent care visit, whereas 54 percent had a scheduled visit with their PCP and 42 percent had a scheduled visit with a specialist they had already met. Among physicians, meanwhile, telehealth adoption spiked among all 20 of the specialties represented in the survey.
The explosion in telehealth use is tapering off somewhat as brick-and-mortar healthcare facilities gradually reopen, but broad utilization of telehealth looks to be here to stay. More than half of all consumers expect to use telehealth more often following COVID-19 than they did before, while 92 percent of providers expect to continue video visits even after it is safe to see patients in person. Physicians and consumers both express a willingness to use telehealth for chronic care check-ins, post-surgery follow-ups, and more — and for many types of visits, patients say they would actually prefer to see a doctor virtually.
Rather than being confined to certain situations or certain types of care, telehealth has become embedded across the full continuum of care. It hasn’t just grown; it is being used in a variety of ways.
Toward a Hybrid Care Model
Consumers, especially, are already used to performing many of life’s activities online. In so many areas of life, the distinction between online and in-person experiences is becoming less and less definitive. We don't think twice about depositing a check online one day and visiting a local bank branch the next. We expect to buy clothes from an online retailer and return them at the store down the street. Now, during COVID-19, patients are scheduling virtual visits with the same doctor they see in person.
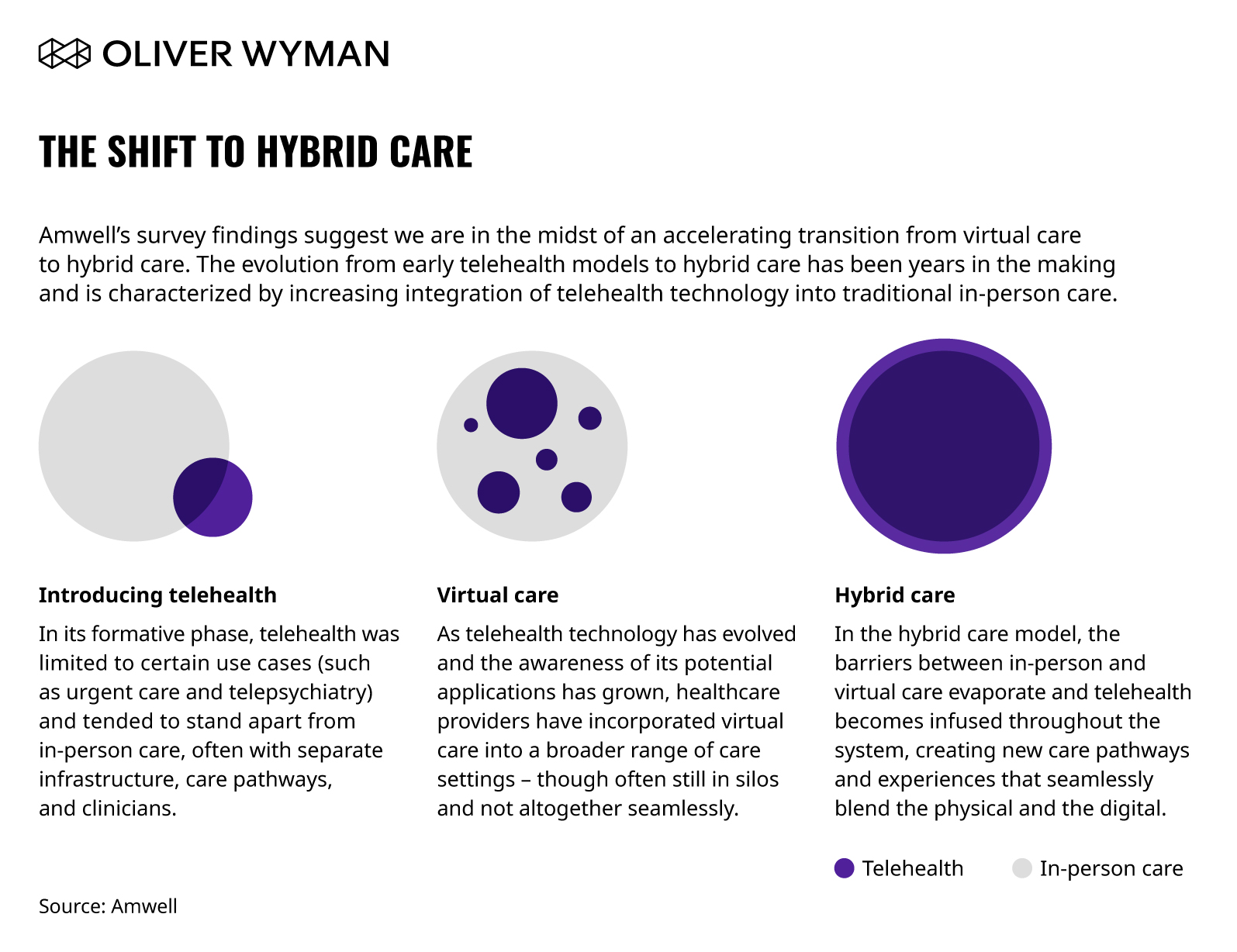
The digital transformation that has reshaped other industries has arrived in healthcare delivery. But what will that future look like? The experience during COVID-19 and the Amwell survey findings suggest we are in the midst of a rapid transition from virtual care to hybrid care.
The term hybrid has taken on new resonance during COVID-19. Parents and teachers talk about hybrid school. Employers are building hybrid workplaces that blend remote work and face time. Hybrid has become part of the vernacular, a useful shorthand for mixing the virtual and the physical.
In healthcare, hybrid care models combine virtual and in-person experiences across the full continuum of care. As patients go through treatment care pathways, in-person elements — procedures, labs, imaging, immunizations — can be seamlessly combined with virtual elements, which might include remote monitoring or a telehealth visit with a specialist from home. Physical encounters still matter, but with hybrid care, the physical joins the digital to create a cohesive experience for providers and patients alike.
The Path Forward
The transition to hybrid care isn't free from obstacles. For instance, while awareness of telehealth has never been higher, our survey found that many consumers are still uncertain about how to identify or access the specific telehealth services available to them through their insurer or PCP. And while the pandemic has eased many long-standing barriers to telehealth adoption among providers, a majority of physicians still cite technology challenges, uncertainty around reimbursement, and questions about clinical appropriateness as barriers to telehealth adoption at their institution.
Building successful hybrid care models will require providers, payers, and innovators to tackle some big questions and challenges:
- Workflows. How will healthcare providers incorporate telehealth and other digital tools into existing clinical workflows in a flexible, sustainable way?
- Workforce. How should health systems optimize their staffing models, training, and talent to anticipate the unique needs of hybrid care?
- Technology. Across the entire healthcare ecosystem, how do we build tools that are interoperable, secure, flexible, and easy to use?
- Engagement and experience. How can providers and payers work together to engage patients and deliver seamless virtual and in-person experiences?
- Capital expenditure. What would a capital budget and a medical campus built around hybrid care look like?
- Policy and regulations. How do we ensure that reimbursement and regulatory changes continue to incentivize models that provide high-quality care at a lower overall cost?
These questions do not have simple solutions. Each organization has its own strategy and priorities. But solutions exist and innovation is occurring. The guiding principles of the hybrid care model are connection, integration, and collaboration — with patient experience and outcomes as the ultimate goals.
Amwell heard clearly from physicians and consumers that they prefer and expect to incorporate telehealth into the existing continuum of care, the experiences and platforms they already know, and the trusted relationships they have with each other. Moving from virtual care to hybrid care will require not only reimagining the delivery of care, but also how the healthcare ecosystem works together to enable that vision.
Editor's Note: For more information, read Amwell's full 2020 survey findings here.