For organizations to successfully transition to a value-based model, they must combine comprehensive population health research with strategic execution. A dash of bold helps, too. When Cornerstone Health Care, a multispecialty group practice in North Carolina, made the decision to pivot from volume to value, they started from the ground up, completely redesigning the care models for their highest-risk patients. In a recent H&HN Daily article, Dr. Grace Terrell, Founder of CHESS (Cornerstone Health Enablement Strategic Solutions) and former president and CEO of Cornerstone Health Care, Dr. Bruce Hamory, Oliver Wyman’s Chief Medical Officer, and Oliver Wyman Partner Josh Michelson detail the “how” of the of the organization's ambitious care-model makeover, and they share the early (and impressive) results.
Cornerstone Health Care was already considered a progressive and successful healthcare organization when they launched their care model redesign initiative. But Cornerstone leadership understood that to keep pace with the shifting healthcare landscape, they needed to shift their fee-for-service sick-care model even closer to a value-based model.
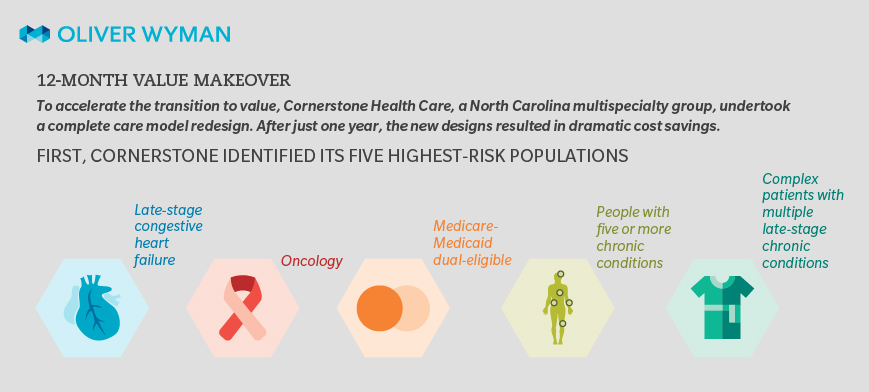
To do that, Cornerstone identified the five highest-risk populations that would impact their overall value: late-stage congestive heart failure, oncology, Medicare-Medicaid dual-eligible patients, those with five or more chronic conditions, and complex patients with multiple late-stage chronic conditions. And instead of shifting resources from other practice areas to impact these groups, Cornerstone wholly redesigned the patient-care model for these five populations. They restructured everything from staffing, care team roles, policies and procedures, and patient engagement methods to the physical layout of offices to create a better patient-care environment. With these changes, coupled with other focused areas of care and specialized programming, Cornerstone was able to significantly reduce patient cost.
Twelve months after the redesign, Cornerstone reported the following results:
- Their transformation program as a whole yielded a nearly 13 percent decrease in total cost of care.
- Some programs achieved savings as high as 19 percent.
- Inpatient hospital costs were reduced by 30 percent.
- Some individual care programs reduced hospitalization by as much as 45 percent.
In the article, the authors stress that this level of transformation is never easy; but the significant cost savings achieved demonstrate the promise and potential of a targeted care model approach.
In the infographic below, Dr. Bruce Hamory and Josh Michelson of Oliver Wyman illustrate Cornerstone Health Care's successful 12-Month Value Makeover.