Editor's Note: This article was originally published in Oliver Wyman's Health Innovation Journal, Volume 3.
In recent years, innovation has vastly increased the number of specialty drugs. There were just 10 specialty drugs on the market in 1990 – by 2008 that number had reached 200 and stood at 300 in 2015. In recent years, more than half of the novel drugs approved by the Food and Drug Administration have been specialty drugs. And more are on the way. Some two-thirds of the pipeline are reportedly specialty. As a class, specialty drugs continue to be expensive, with some new therapies priced at unprecedented levels. For example, a one-dose therapy course of Zolgensma, a recently approved gene therapy for spinal muscular atrophy, will cost up to $2 million. Meanwhile, specialty drugs have moved beyond cancer and orphan diseases and now target some much more common conditions, like eczema and certain kinds of asthma.
Specialty drugs increasingly constitute a greater share of the nation’s prescription drug spend. Specialty spending has reportedly risen $255 per person since 2009, even as spending on traditional net medications has decreased by more than $210 per person. Specialty medicines accounted for just under half of per person drug spending in the US last year ($517 of $1,044 total), and it’s projected they will make up more than half of all US drug spending this year.
Specialty Growth Is Here To Stay - Let's Embrace New Approaches
Specialty drugs offer new hope for a growing portion of the population grappling with difficult conditions. These powerful drugs are some patients’ only options, worth the price of life no matter how costly in the short term. While a high-cost specialty drug regimen that cures a chronic patient may be less costly on a long-term basis when compared to ongoing disease treatment, these near-term costs place strains on an already unsustainably expensive healthcare system. Novel approaches are required to navigate the rising tide of specialty drug costs. Traditional tools like formulary placement, prior authorization, and step therapy will still be necessary, but won’t be enough to manage utilization of today’s very diverse, very targeted, and very expensive specialty medications and the moral population health dilemmas they present.
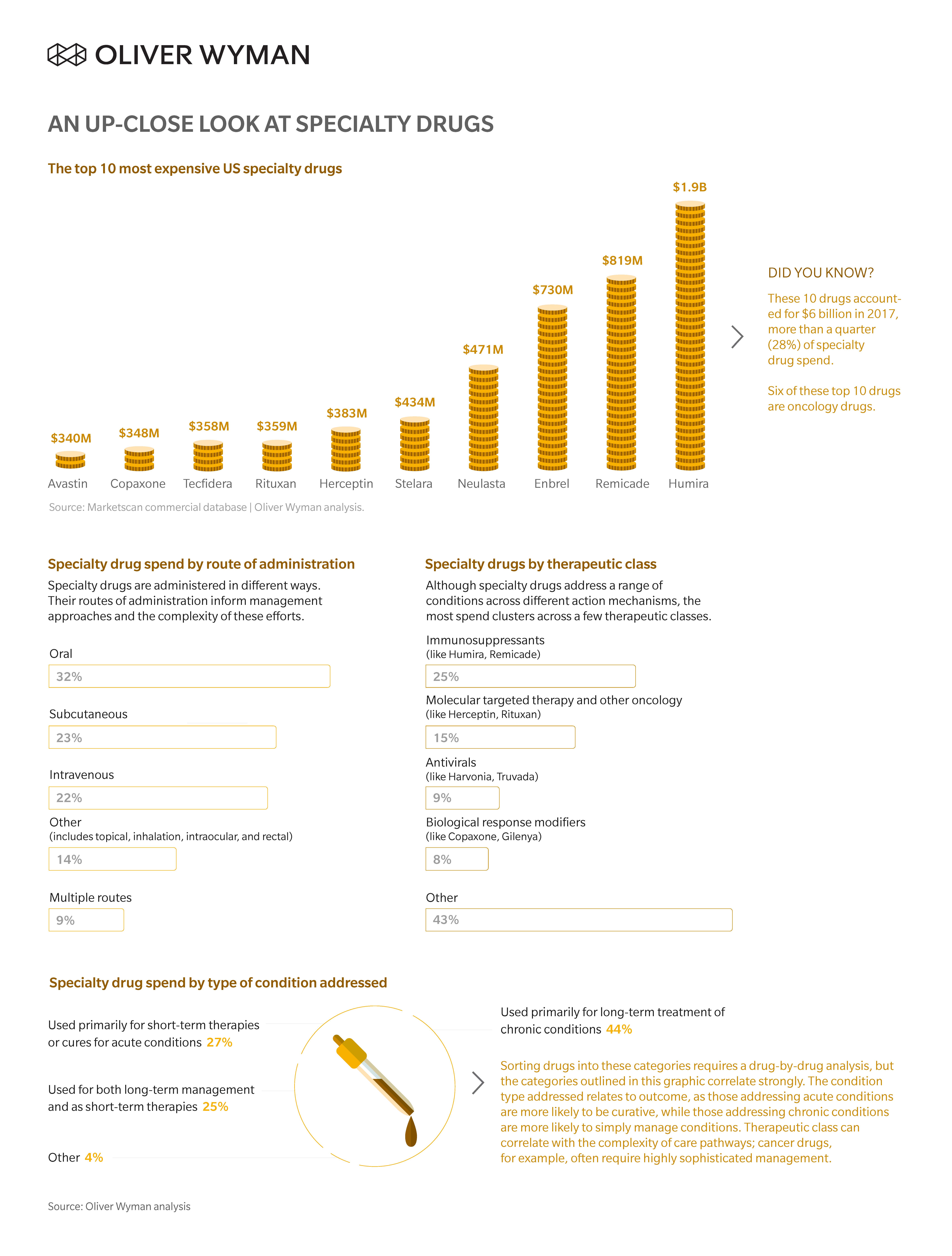
The cost is concentrated. The specialty category encompasses a range of high-cost drugs. However, there are standouts, even within this expensive class. Within the nearly 3,500 therapies we classify as specialty, the top 10 drugs make up approximately 25 percent of costs, and the top 50 drugs make up over half of costs. This pharmacy “population cost pyramid” is resonant of the commonly cited medical population cost pyramid where five percent of the population drives 50 percent of the costs. However, this pyramid is driven by a very different profile of conditions and patients now driving these costs. Effectively managing specialty pharmacy requires specific focus on these high-cost drugs – a focus that incorporates purpose-driven management approaches.
A Unique Management Approach
Specialty drugs fall into a wide range of therapeutic classes. For instance, there are maintenance drugs and one-course cures. There are drugs requiring significant management by expert clinicians and those that patients can self-administer with autonomy. There are drugs that offer the only alternative for patients with life threatening conditions, and others part of the armamentarium for conditions already well served.
When it comes to managing specialty drugs’ outcomes and costs, traditional approaches typically orient around therapeutic classes, which makes sense. However, another way to ensure the appropriate management approach is to align it around a combination of outcomes the drug therapy seeks to achieve and the complexity of the overall patient-care pathways. From this lens, there are three major categories to consider:
1. HIGH-COST, ONE-COURSE CURES
This archetype contains drugs that are extremely high-cost, one-course cures for complex conditions. Examples are Zolgensma, which treats spinal muscular dystrophy, and Harvoni, the Hepatitis C cure. These drugs also present some of the greatest moral dilemmas, as just a few patients receiving these treatments can drastically impact self-funded employer group or health plan costs – ultimately leading to increases in healthcare costs and premiums for all. Payers, providers, and manufacturers must closely collaborate to ensure these drugs are the most appropriate and best course of action for patients weighing both short- and long-term impacts. Balancing the application of a new curative therapy approach versus the continued use of a condition management therapy approach can be a difficult decision requiring deep clinical and population health expertise. With the rise of these types of curative regimens expected, additional focus, processes, and skills will be needed to navigate the issues around formulary coverage, pricing, and clinical approvals.
2. CHRONIC CONDITION MANAGEMENT
A second category consists of drugs used regularly over a long period of time to manage chronic conditions (and sometimes effectively cure them over an extended period). Effective engagement between patients and providers is critical for these drugs. Patient adherence ensures the drugs’ benefits are realized. Even more critical? A highly coordinated patient care approach, as these drugs may require that a patient, for example, adhere to a strict diet, take a course of other medications to manage additional conditions or side effects, and faithfully report progress back to their physician. This calls for a synchronized approach to managing the patient’s care across medical, behavioral, and pharmacy care aspects – something a focus on reducing specialty drug costs alone will miss. Value-based health models that align providers with total cost and care outcomes are appropriate tools for this category. It’s also critical administration occurs at the appropriate place, that patients have accessibility to their overall drug regimen, and that patients’ social determinants of health are taken into account.
3. ACUTE CONDITION MANAGEMENT
A third category includes drugs used as needed for the episodic management of an acute condition such as cancer. These drugs are complex to manage. They generally must be administered on-site and are often tangled with moral and ethical considerations around patient preferences, quality of life, and life extension. Traditional management techniques, like prior authorization, are certainly necessary but unlikely to have a significant effect on spending unless applied before the patient begins a course of treatment. Managing these drugs requires a holistic approach where clinicians are engaged, and therefore more likely to follow the right care pathways to effectively manage side effects, attend to patients’ full set of health needs, and transition therapies as appropriate, including intensive patient and caregiver support to help navigate difficult health and lifestyle decisions.
Our Call To Leaders: Integrate More Within These Three Catagories
Managing the first drug category requires a predictable set of levers, ensuring patients are truly good candidates for the drugs they’re prescribed, carefully setting dosing and course, and delivering drugs in the most effective setting (which can be at times in the home). The second category of drugs requires more complex management, integrating careful monitoring of the drug itself with numerous other healthcare and broader lifestyle facets necessary to ensure the drug accomplishes its goals and that adverse outcomes are avoided. The third category of drugs requires especially tight payer-provider communication to ensure the right therapies are applied and managed in the context of patients’ other health needs. Ultimately, all three categories require a more integrated approach to care and costs – something that’s historically been managed in a more siloed way within most payer organizations.
Today’s (and tomorrow’s) specialty drugs represent a massive opportunity to better serve patients. But they also pose serious risks to individual payer and self-funded employer group economics, and the healthcare system at large if pricing strategies and cost management aren't effectively navigated. They require a more active, specified, and integrated approach to both medical and specialty-drug management, one that requires purpose-built approaches incorporating provider partners, close collaboration with members/patients, and engagement in alternative reimbursement approaches alongside typical utilization management techniques. The goal is nothing short of ensuring that the remarkable achievements of medical science benefit patients – without destroying the healthcare system that serves them along the way.