EDITOR'S NOTE: Oliver Wyman recently facilitated a Briefing Room discussion with leaders from Health Evolution, American Express, Blue Cross and Blue Shield of Louisiana, and Allina Health at the 2019 Health Evolution Summit in Dana Point, California. During this discussion about how artificial intelligence is transforming healthcare, panelists from both in and out of healthcare shared their views before an audience of payers, providers, and life science chief executive officers to help push technology solutions beyond traditional boundaries. Below is a summary of key takeaways from this panel, as published in a joint report written by Health Evolution and Oliver Wyman, and also in the third edition of the Oliver Wyman Health Innovation Journal.
After decades of being considered futuristic, Artificial Intelligence (AI) is getting real in healthcare for customer experience, care management, and cost competencies, among other use cases. Smart payers, providers, and life sciences organizations, in fact, are looking across industries to learn from companies that have already implemented AI to reap impressive results.
To that end, leaders from all sectors of healthcare came together for this year’s Briefing Room at the 2019 Health Evolution Summit to discuss how AI is transforming healthcare and to learn from the experience of Ash Gupta, an industry pioneer in transforming traditional analytics to big data and AI.
American Express, for its part, can now process ten billion transactions annually and detect fraudulent claims in under ten milliseconds – a degree of efficiency and precision many in health care are striving to achieve as they integrate AI inside and outside of clinics.
Against the backdrop of three major trends that signal where the industry is headed, nine steps to successful AI in healthcare emerged from the discussion. We’ll delve into each as well as address a few key future workforce considerations.
AI IS CHANGING THE LANDSCAPE
Based on insights shared in the Briefing Room, leaders pointed to three major shifts propelling exponential growth in healthcare’s data analysis and processing capabilities.
1. First, the world is producing more (and much better) data than ever before. Over two trillion gigabytes of healthcare data are anticipated to be produced in 2020 alone, and this rate will continue to increase as healthcare data is projected to have a compounding annual growth rate of 36 percent into 2025.
2. AI-based source algorithms and cloud-based data lakes allow healthcare and other players to analyze data in ways previously unimaginable. Leaders pointed to how at American Express, for instance, queries once taking 120 days to complete now take 10 minutes or less. Quarterly endeavors have become daily tasks.
3. The third major shift is that more quantitative scholars (like mathematicians) opt to go into the private sector instead of academia; a reported one in two university-hired scientists leave academia after only five years. People are entering fields that didn’t even exist a few years ago–like AI and computational science.
STRATEGIES FOR AI SUCCESS IN HEALTHCARE
1. Embed big data and AI into your company’s DNA. Success requires executives to develop an informed understanding of AI and big data like they know their customers, products, and profit and loss statements. Moreover, managing a dynamic strategy requires healthcare leaders to understand the possibilities and limitations of technology underpinning future transformation.
Gupta shared that in order to understand the AI landscape, top executives in his team traveled to different parts of the world to interact with technology startups. “For two days, we would listen to see what types of problems they were trying to solve and how our use cases related to them,” added Gupta. “We learned many things while touring the world, including: how new data sources like mobile, IP addresses, and bank statements might increase our informed understanding of customer need; how offline and online matching algorithms provide a 360° customer view to provide multi-channel marketing; how to build best-in-class data lakes and AI-based models while optimizing computing capacity; and how to turn analytics into production with minimal lag time.” Healthcare CEOs agreed that in the future, they will likely be part of the problem-solving exercise rather than merely delegate this to information technology or analytics experts.
2. Invest in talent. Data transformation does not require hiring an entirely new workforce. Gupta believes 85 percent of employees working on data and analytics can be trained to build and leverage new techniques. However, for 15 percent, the right programs had to be established to ensure we recruited people “born” on big data and AI as catalytic agents of change. We need to create mechanisms as well, so people can reach cruising speed quickly. Leaders agreed that high turnover rates are not just a healthcare problem, and discussed that even Facebook employees leave after an average of two years. Why? According to Facebook’s Human Resources team, their employees reported it wasn’t because of bad bosses, but bad jobs.
For Steve Udvarhelyi, MD, President & CEO at Blue Cross and Blue Shield of Louisiana, the transition to big data is more of a talent and organizational effectiveness problem than a technical challenge. “My biggest worry is whether the people running the business have the right questions to ask,” he said.
3. Foster innovation. Innovation must become a grassroots movement, something that happens from both the top down and bottom up. Employees should feel empowered when problems and encouraged to take risks (and take risks often). Gupta emphasized, “The only weakness in our system is your imagination.” With the advent of cloud, open source AI-based modeling techniques, and vastly available new, cheap talent, it’s possible to analyze and execute on ideas that would historically take long lead times and cost. Plus, the new technology allows you to test and learn, thus rapidly arriving at a best-in-case solution. Three specific solutions are: 1) Evaluating a target list of customers for product upgrades; 2) Analyzing customer complaint data without human bias to improve servicing; 3) Analyzing customer calls to determine impending economic weakness.
4. Avoid the fear of failure. Failure is an inherent part of driving innovation. “When I doubted the project, the goal was not to prove them wrong. The goal was to prove myself wrong,” Gupta said of his experience greenlighting projects. In the Briefing Room, progressive healthcare leaders said they are also testing pilots knowing many of them might fail. “If you’re not failing, you’re not innovating enough,” emphasized Ron Williams, Aetna’s former Chairman and CEO.
5. Implement, test, refine…repeat. Home runs don’t happen on day one. Initial results are almost always worse than existing practices. A Briefing Room member shared how the first model predicting risk said, “late-stage kidney disease patients are going to be high-cost.” Not exactly revolutionary findings. At American Express, an early predictive model indicated that more line credit should be given to everyone–more line credit, more revenue, it reasoned. However, the algorithm failed to recognize the increased risk. “Leaders must engage business and analytics with the understanding that business knowledge comes first,” said Udvarhelyi. “You need to test and learn so the outcome gets better.”
When faced with high stakes and an aversion to change, algorithms should run in the background and offer suggestions while stakeholders make the final determinations. The first time AI suggests a solution, experts’ decisions will likely be better than those suggested by algorithms. In fact, the best results require collaboration between machines and humans. PathAI – a company looking to automate the time a pathologist spends reading slides – boasts a 2.9 percent error for the algorithm alone (compared to 3.5 percent error for pathologists). When combined with human input, however, the error rate drops to 0.5 percent.
6. Collaborate. Briefing Room members agreed healthcare players must continue to develop effective industry consortiums (a la Argonaut and Da Vinci). In finance, competitive entities share information for which IP addresses represent fraudulent accounts and should not be approved for credit cards. Players entering information into the pool benefit from collective common knowledge and network economics pay large dividends. Success requires collaboration and healthcare is rising to the challenge. The Da Vinci and Argonaut projects have enormous potential to turn isolated data into better outcomes and lower costs. Gupta also encouraged collaboration. “You have a lot of data silos you want to turn into a cloud-based data lake,” he said. Data should serve as a corporate asset, not the property of each company department, Gupta added. This is the only way to stitch data across disciplines (like marketing, servicing, and risk), across channels (like online and offline), and across businesses and geographies. He emphasized that controls are obviously necessary so use is “permissible” and in customers’ best interests. This way, your data asset becomes clean and free of error and can be leveraged by data scientists and decision- makers rapidly and innovatively. The advent of cloud, hard commodities, and open source has created big data lakes where providing great cost/benefit gain comes at a reasonable price. Looking beyond clinical data, Penny Wheeler, MD, President & CEO at Allina Health, urged members to collaborate on data that goes beyond traditional sources, including social determinants of health. “Electronic medical record data is not enough,” she stressed. Collaboration, of course, does not end at data alone…in fact, it transcends the entire ecosystem, including analytics and execution.”
7. Be transparent. The infamous Black Box, and its inability to explain algorithm results, occurs across industries. At American Express, every algorithm had to be able to give a plain-English explanation of why decisions were made, shared Gupta. “The adverse effect of an algorithm error is much larger in healthcare than in other industries,” said Rod Hochman, President and CEO at Providence St. Joseph. Algorithms must produce transparent answers that can easily be traced and explained. Briefing Room members agreed that healthcare leaders must not create opaqueness in the system.
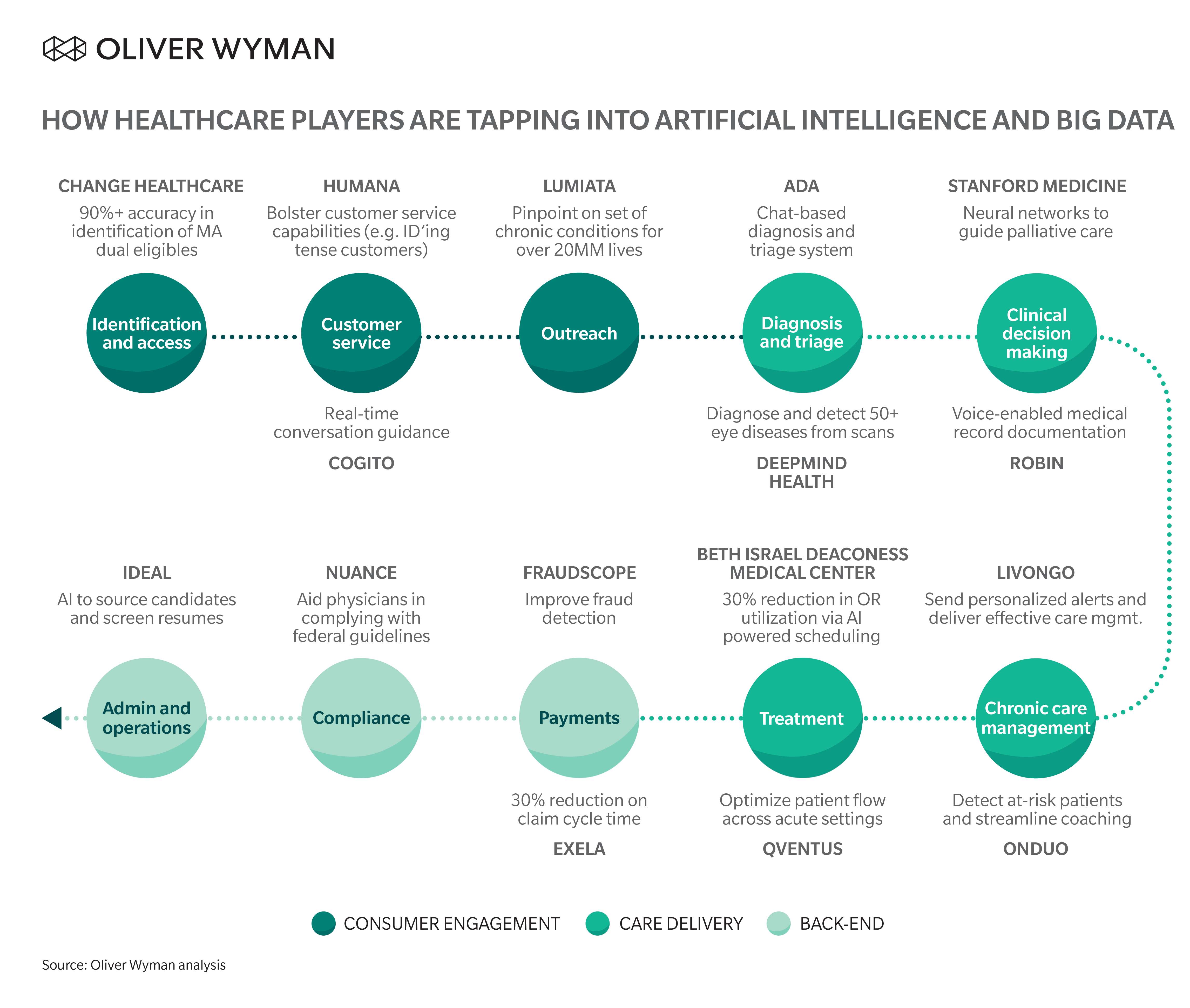
EXHIBIT 1
8. Keep customers front and center. Healthcare leaders agreed that they need to consider what matters most to customers as much as possible. As more data is generated and collected, permissible use of data and focus on information security will play a big role. To foster customer trust, Gupta advised leaders to explain how data is being used in a way that is advantageous to their own needs. Ideally, customers should be thankful their data is in your hands.
9. Use everything you have. Start yesterday, was one of Gupta’s main takeaways, and healthcare leaders around the room agreed. Innovative players are quickly turning existing data into analysis. Every piece of data collected should be utilized. New hires and existing teams should immediately focus on creating insights. Udvarhelyi said physicians don’t need more data, but they do need more wisdom. “We need to blend business knowledge with analytics now,” he urged.
PLANNING FOR THE FUTURE WORKFORCE
With so many changes coming on the horizon, healthcare CEOs are already forecasting new workplace needs in the next three to five years.
Seventy percent of healthcare leaders believe data is essential for growth and to improve consumer experience – and 54 percent believe widespread AI adoption is fewer than five years away.
Leaders emphasized how AI is making big waves across the industry. Alphabet’s DeepMind detects gender through eye scans. Mount Sinai’s Icahn Institute trained an algorithm on electronic medical record data to predict the onset of schizophrenia. FDA-approved Lucid Robotic uses AI to detect potential clots in stroke patients. And those are just three examples.
The landscape is changing. Healthcare organizations will need new skill sets to keep pace. Embracing the strategies outlined in this report will lay a strong foundation for the AI-ready workforce of the future.